|
11/28/2018 1 Comment Dr. Karen Shelton Performs Central Alabama's First Xen Gel Minimally Invasive Glaucoma StentWe are always excited to lead the way in offering advanced procedures for your patients. Last week, Dr. Karen Shelton performed the first Xen Gel Minimally Invasive Glaucoma Stent in central Alabama.
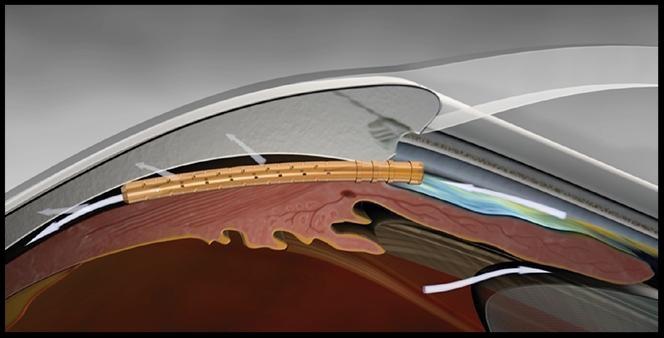
We sat down with Dr. Shelton to get her thoughts on the Xen and discuss the procedure. What are some of the key benefits that Xen Gel Stents offer our glaucoma patients? As you probably know, XEN was first Launched in 2017 following FDA approval in November 2016. It is the only approved MIG device that allows for subconjunctival filtration.
1 Comment
In the conversations leading up to our recent burnout panel (Click here to watch!), we noticed a common phrase being used: "I don't manage my staff; they manage me!"
There are many factors that contribute to burnout, but perhaps an unexpected culprit is the lack of control many doctors feel in their own practices. Who is really in charge while you are scrambling from exam room to exam room all day? When you don't set the schedule, handle the financials, or manage the employees, it is easy to feel like an employee yourself. As this process plays out day after day or over even over years, the tendency for many doctors is to become (or at least feel) like they are just a cog in the system. We are less than one month away from our annual December CE!
Please join us on Saturday, December 8th at our VisionAmerica Birmingham Campus for four hours of great continuing education. The CE will begin at 9:00 a.m. and will last until 1:00 p.m.! The cost of attending the CE is a minimum of $100 (tax-deductible) and all proceeds will benefit Altar 84, which is a local non-profit involved in orphan care. Payment can be made via PayPal on the link below or by check. Dr. Rod Nowakowski will be speaking on Genetic Testing in Macular Degeneration and Dr. Karen Shelton will lecture on Surgical Options in Glaucoma. Dr. Michael Eddins will also be sharing some thoughts on advances in cataract surgery. More details will be made available soon. Go ahead and mark your calendars! Please click here to sign up for the CE! by Rod Nowakowski, OD, PhD
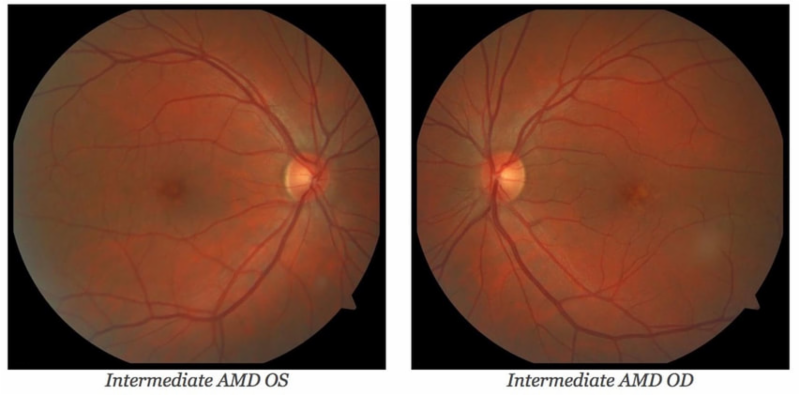
Genetic & Advanced Diagnostic Testing Disclosures 1. I have no financial or other interest in any company or product referenced in this article. 2. This is a follow-up to the case Dr. Batson presented in a previous email involving a 54-year-old woman who developed prominent macular drusen observed to increase in number and size over 1 year. (Click here to read Dr. Batson's piece.) 3. Thank you to those of you who posed questions about his case and the related genetic testing. Some are answered below and others may be addressed later. 4. This is a summary of a complex topic and is missing a lot of detail that you can find in various references. Why you should read this! "The AREDS formulation modifies the risk of progression to NV [neovascular AMD] based on individual genetics. Its use should be based on patient-specific genotype." (Click here to read more!) Introduction As you are probably aware, on August 29th, 2018, Alcon voluntarily withdrew the CyPass device due to safety concerns based on five-year data. The concerns centered around a higher rate of endothelial cell loss in patients receiving cataract surgery plus CyPass compared to cataract surgery alone. Overview of Results
At five years, patients undergoing cataract surgery with CyPass demonstrated a 20.5% loss of endothelial cells vs. 10% in the control or cataract surgery only group (of note, the control group was unusually low compared to other published data). There appears to be a correlation between CyPass implantation depth and rate of endothelial cell loss. For eyes with:
Of note, early migration of the CyPass device has been reported and, according to the Preliminary ASCRS CyPass Withdrawal Consensus Statement, "the potential for migration remains an important variable to be considered for long-term diagnostic monitoring". What does this mean and what should I do for my patients with CyPass? It's important to remember a few pertinent points. One, most of the endothelial cell loss did not occur until year four and five so it may be a while before we were to see any potential complications. Two, although certainly a risk factor, not everyone with endothelial cell loss will develop corneal edema. Three, removal or repositioning of a CyPass without the presence of corneal decompensation is likely to cause further endothelial cell loss. The current recommendations for monitoring patients should include:
Monitoring these patients with clinical examination at standard glaucoma follow ups should be adequate. We are always happy to monitor and evaluate patients as needed. Any evidence or concern for corneal decompensation should be referred back to the surgeon for further evaluation. Speaking of the CyPass withdrawal, VisionAmerica's glaucoma specialist, Dr. Karen Shelton noted, "For a minimally invasive procedure, CyPass provided a great response for many patients. I hated to see it withdrawn but understand the concerns. I don't anticipate having to remove or manipulate previously inserted devices unless we start to see corneal changes." If you have any questions or concerns, please don't hesitate to give us a call. |
AuthorThe staff and doctors at VisionAmerica are committed to providing relevant information for you, your patients and your practice. We hope you find the information in our blog post helpful. Archives
August 2019
Categories |

 RSS Feed
RSS Feed
