|
(As we have in the past, we want to continue to share challenging cases that arise in our day-to-day practice. The article below from Dr. Batson is a recap of one of his recent interesting cases.) Symptoms A 61 year old female presented with complaints of intermittent "aura" with blurring of colors in her central vision. Her symptoms occur multiple times throughout the day with no associated pain or headaches. Previous History Medical History: migraine headaches and rheumatoid arthritis. Past Ocular History: Cataract surgery Social History: Former smoker Medications: duloxetine, estradiol-norethindrone, folic acid, levocetririzine, methotrexate, nabumetone, plaquenil, polyethylene glycol and progesterone. Allergies: None Review of systems: Positive for difficulty hearing, anxiety, joint pain/swelling and easy bruising Base Exam Findings Uncorrected Visual Acuity OD 20/25-1 OS 20/20-2 Confrontation Visual Fields - full OU EOMs - normal with no pain on eye movement Pupils - normal with no APD IOP - 16mmHg OU Anterior Segment Findings Lids / LashesNormal OU ConjunctivaNormal OU CorneaNormal OU ACDeep and Quiet OU IrisNormal OU LensPCIOL Centered OU with clear PC Dilated Fundus Examination NerveC/D .3 OU with normal color and contour MaculaNormal OU Vessels Normal OU PeripheryNormal OU with no tears, holes or detachments VitreousNormal OU with no PVD seen Differential Diagnosis The differential for this patient includes the following:
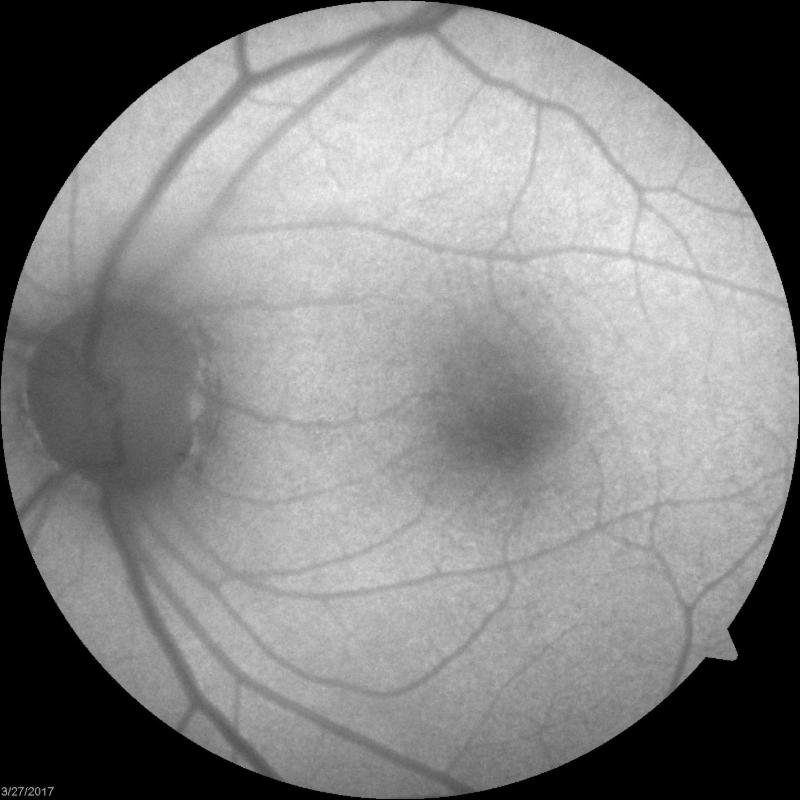
Diagnostic Testing The diagnostic testing for the patient revealed the following:
Diagnosis
Plaquenil retinal toxicity. My differential diagnosis list included several other potential etiologies. The frequency of symptoms (multiple times throughout the day) would be unusual for migraine with aura. While vitreous opacities is a possibility, there were none seen on clinical examination. Retrobulbar optic neuritis is also a consideration but there was no pain on eye movement and a bilateral simultaneous presentation would be extremely unusual. In this case, the diagnostic testing helped to solidify the diagnosis. The paracentral ring scotoma on VF, perifoveal loss of IS/OS photoreceptor layer on SD-OCT and diminished response on mfERG are all consistent with Plaquenil retinal toxicity. In this particular case, the patient had a 14-year history of Plaquenil for rheumatoid arthritis. Management The Plaquenil was immediately discontinued. In addition, correspondence and copies of the diagnostic testing were sent to her rheumatologist. A follow-up examination was scheduled for three months. Discussion/Challenges Hydroxychloroquine (Plaquenil) has been used for many years to treat conditions such as malaria, rheumatoid arthritis and lupus. Initially thought to be rare, a recent study found a prevalence of 7.5% with varying dosing and duration but increased to 20% with a duration greater than 10 years. (1) 1 Dosing and duration seem to be the primary risk factors. According the the most recent American Academy of Ophthalmology Recommendations on Screening for Chloroquine and Hydroychloroquine Retinopathy - 2016, "The risk of toxicity is dependent on daily dose and duration of use. At recommended doses, the risk of toxicity up to 5 years is under 1% and up to 10 years is under 2%, but it rises to almost 20% after 20 years." (2) The most recent screening recommendations from the same paper (click here) are as follows: Baseline Screening
Take Home Message
(1) Melles RB, Marmor MF. The risk of toxic retinopathy in patients on long-term hydroxychloroquine therapy. JAMA Ophthalmol 2014;132:1453-60. (2) Marmor MF, Kellner U, Lai TY, Lyons JS, Melles RB, Mieler WF: Recommendations on screening for chloroquine and hydroxychloroquine retinopathy (2016 Revision). Ophthalmology 2016, 123:1386-1394.
0 Comments
Leave a Reply. |
AuthorThe staff and doctors at VisionAmerica are committed to providing relevant information for you, your patients and your practice. We hope you find the information in our blog post helpful. Archives
August 2019
Categories |











 RSS Feed
RSS Feed
